Courtnet Pandolfi, de Garden Grove, se declaró culpable en febrero del asesinato de Yesenia Aguilar. Tambien se...
Salud Mental
Salud Mental
Hoy 1 de abril entra en vigor la ley del consumo recreativo de cannabis en Alemania. La...
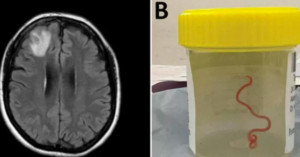
Una mujer australiana de 64 años se sometió a una operación cerebral sin saber que albergaba un...
En Colombia, el sector sanitario está en alerta máxima ante el creciente número de jóvenes que se...
The global opioid epidemic has had devastating consequences on communities around the world, with the United States...